Estimated reading time: 6 minutes
Many of us expect our menstrual cycles to arrive like clockwork. But what happens when they don’t? When they’re early, late, heavier, lighter or simply different from what you’re used to?
Understanding what constitutes a truly irregular period, what’s behind it, and what you can do about it is more than health-curiosity, it’s essential to your well-being.
Drawing from credible sources like Cleveland Clinic, Medical News Today, National Institute of Child Health and Human Development (NICHD) and the National Health Service (UK), this article takes a fresh, holistic look at irregular periods, what they mean, why they happen, and how you can respond with clarity and purpose.
What do we mean by “irregular periods”?
Let’s start with the baseline. A typical menstrual cycle is about 21 to 35 days long, with bleeding lasting roughly 4 to 7 days.
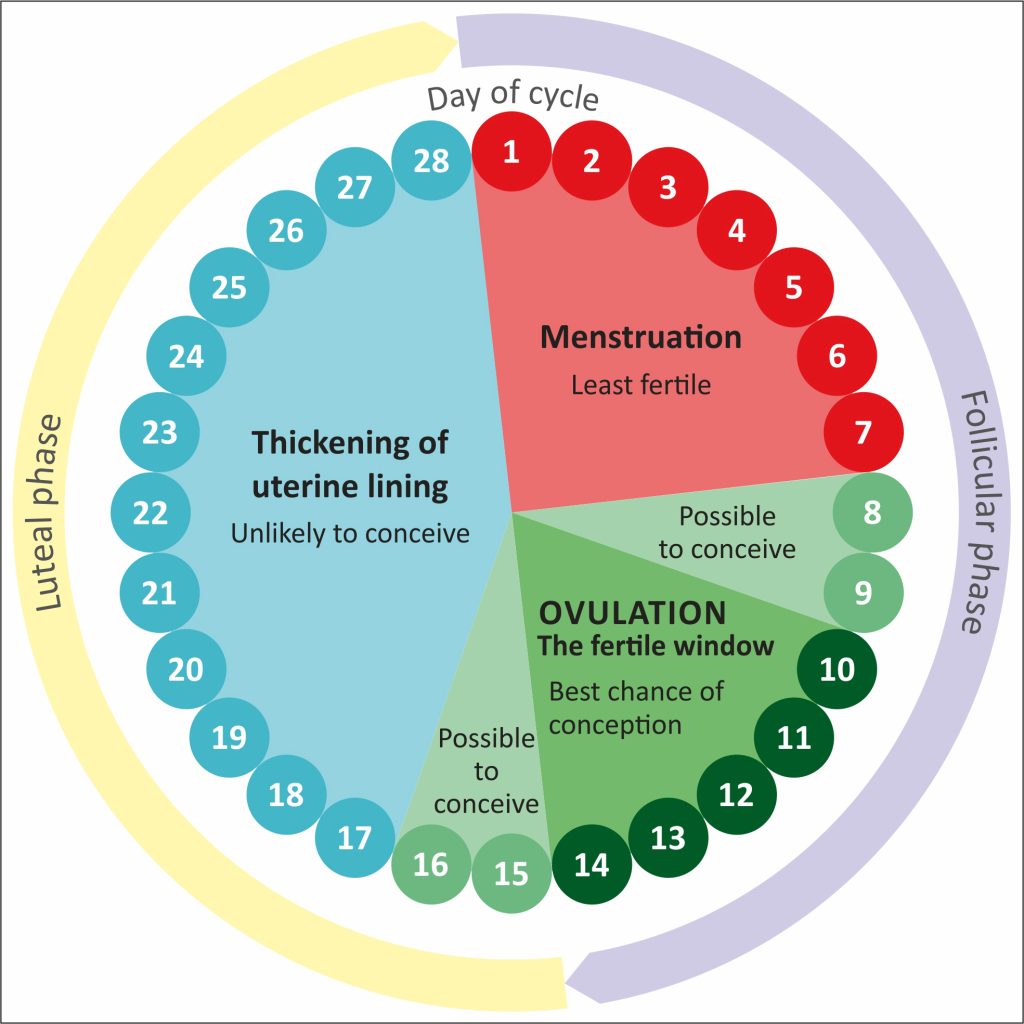
- Here are some examples of Irregular Period:
- Periods fewer than 21 days apart, or more than 35 days apart.
- Missing three or more cycles in a row (when not pregnant, breastfeeding or menopausal).
- Bleeding that is much heavier or lighter than usual, or that lasts longer than seven days.
- Flow that varies widely from one cycle to the next (difference of more than nine days between cycles).
So, if your cycle used to be roughly 28 days and now, you’re seeing 45-day gaps, skipped months, or very heavy bleeding, it’s a clearer sign something is up.

Why does your cycle go off script?
The menstrual cycle is a finely tuned hormonal symphony: estrogen, progesterone, luteinizing hormone (LH) and follicle-stimulating hormone (FSH) all play coordinated roles.
When that balance is disrupted, the rhythm shifts.
Below are major categories of causes—with real life relevance and actionable notes.
a) Lifestyle and external factors
Stress: High levels of emotional or physical stress raise cortisol and adrenaline, which in turn can suppress ovulation and extend or disrupt your cycle.
Weight change / exercise extremes: Rapid weight loss or gain, low body fat (especially in athletes or dancers), or excessive training can upset hormonal signals.
Medications / contraceptives: Starting, stopping or changing hormonal birth control can lead to spotting, missing periods, or heavier/lighter flow.
b) Common underlying health conditions
Polycystic Ovary Syndrome (PCOS): One of the top culprits. PCOS disrupts ovulation, elevates androgens, and often presents with irregular or absent periods.
Thyroid dysfunction: Both hypothyroidism (underactive) and hyperthyroidism (overactive) can affect cycle length, heaviness and regularity.
Structural or reproductive organ issues: Conditions like Endometriosis, uterine fibroids or pelvic inflammatory disease (PID) can cause bleeding between periods, heavy flow, or missed periods.
Hormonal insufficiencies: E.g., primary ovarian insufficiency, pituitary or hypothalamus disorders.
c) Natural life-stage shifts
Adolescence: The first few years after menstruation starts often show variation as the cycle matures.
Perimenopause: Approaching menopause, your hormonal environment changes, cycles may shorten, lengthen, skip or become erratic.
Why it matters: beyond a “just annoying” period
An irregular period isn’t just inconvenient; it can signal deeper issues. Here’s why paying attention is worth it:
- Fertility & conception matters: If cycles are unpredictable, it can affect ovulation timing and impact chances of conceiving.
- Underlying health signals: Persistently heavy bleeding could lead to anemia; abnormal spotting may point to infections or (rarely) early cancers.
- Holistic health link: Your cycle reflects more than the reproductive system—it interacts with thyroid, metabolic, mental health and bone health systems.
When to seek medical support? If you’re experiencing any of the following:
- Bleeding so heavy you’re changing pads/tampons every hour for several hours.
- Spotting between periods, or after sex.
- Skipping multiple periods and not pregnant, breastfeeding or menopausal.
- Sudden dramatic change in menstrual pattern.
What you can do: proactive steps & how to respond
Here is a three-tier strategy: track → understand → act.
Track your cycle intelligently
Use an app, calendar or journal to note:
- First day of menstrual bleeding
- Last day of bleeding
- Duration and heaviness of flow (e.g., heavy enough to soak through pad/tampon in an hour)
- Symptoms: cramps, mid-cycle spotting, mood changes, fatigue
- Significant lifestyle events: stress, weight change, new exercise regimen, medication changes
With repeated tracking you’ll build a baseline for your normal—and hence spot significant shifts more clearly.
Lifestyle optimization
Stress management: Try mindfulness, meditation, proper sleep. Chronic stress is a known disruptor of the cycle.
Balanced nutrition & stable weight: Try to avoid extreme diets or sudden weight changes. Your body needs hormonal fuel.
Exercise smartly: If you’re an athlete or training intensely, make sure calorie intake is sufficient and body is getting rest.
Routine check-ups: Doc visits for thyroid, hormonal, reproductive health depending on your risk/age.
When to seek professional help
If your tracking reveals worrying signs (see section above) or you’re trying to conceive and cycles are irregular, it’s time to see a health professional. They may order:
- Blood tests (hormones, thyroid, prolactin)
- Ultrasound to check for structural issues (e.g., fibroids, polyps)
- Examination of contraception / medications you’re using
- Referral to a specialist if needed (gynecologist, endocrinologist)
- Treatment could involve medications (hormonal contraception, thyroid meds, PCOS management), lifestyle interventions or in some cases surgical options (e.g., fibroid removal)
Trying Herbal Supplements for Hormonal Balance
If you prefer a natural approach, incorporating herbal supplements can be a gentle yet effective way to support cycle regularity.
Certain herbs have been traditionally used to nourish the reproductive system, balance hormones, and ease menstrual discomfort. Blends containing ingredients like vitex (chasteberry), dong quai, red raspberry leaf, maca root, Jamaican dog blood, or sarsaparilla are known to promote hormonal harmony and healthier ovulation patterns.
At The Healthy Woman, we craft formulas that target specific concerns such as fibroids, PCOS, blocked tubes, and irregular cycles, combining herbs that works to cleanse, tone, and rejuvenate the womb.
Our Fertility and PCOS Support Capsules, Fibroid Fighter Capsules, and Hormonal Balance Drops are designed to help your body find its rhythm again, naturally.
Of course, while herbal support can make a real difference, it’s important to pair it with proper nutrition, hydration, and rest for the best results.
Always check with a qualified health practitioner before beginning any new supplement regimen, especially if you have existing conditions or are on medication.
Final thoughts: Listen to the rhythm, don’t dismiss the cue
Your period isn’t just a monthly inconvenience; it’s a biological messenger. When it deviates from your personal “normal”, it’s your body’s way of saying something’s changed.
By tracking thoughtfully, maintaining a supportive lifestyle, and seeking help when needed, you give yourself the best chance of staying in tune.
Don’t simply accept unpredictability as the new normal. With knowledge, you reclaim power.
Remember: If you experience any alarming symptoms, such as very heavy bleeding, clotting, missing months without reason, or bleeding after menopause, seek medical attention. This article is for informational purposes only and does not replace personalized medical advice.
Here’s to clearer cycles, stronger insights, and a more empowered brand presence built on genuine value.








