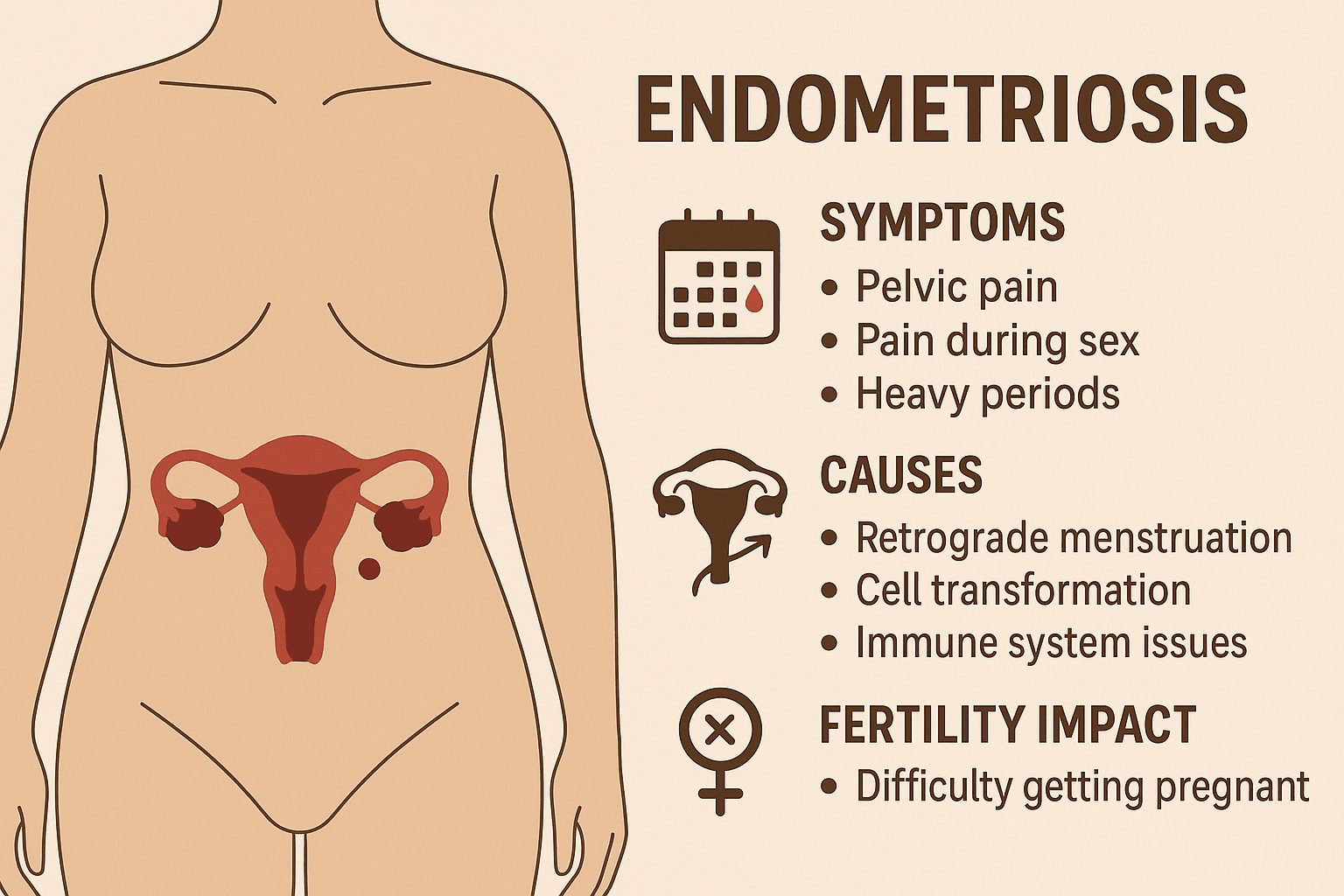
Endometriosis is one of the most misunderstood conditions affecting women with a uterus. Many suffer for years before getting answers, often believing their pain is “normal.” In reality, endometriosis is a medical condition with clear symptoms, known causes, and effective treatment routes, but because awareness is still lacking, millions remain undiagnosed.
This guide breaks everything down in simple and direct language. No medical confusion. No overwhelming jargon. Just real information you can finally understand.
What Is Endometriosis?
Endometriosis happens when tissue similar to the lining inside the uterus (the endometrium) starts growing outside the uterus.
This abnormal tissue growth is commonly found on:
- Ovaries
- Fallopian tubes
- Pelvic walls
- The outside of the uterus
- Bladder
- Intestines
Even though this tissue is not exactly the same as uterine lining, it behaves similarly. It thickens, breaks down, and bleeds with each menstrual cycle, but since the blood has nowhere to exit, it causes:
- Irritation
- Inflammation
- Scar tissue
- Adhesions (organs sticking together)
- Cysts (endometriomas)
This is why the pain can feel deep, sharp, and unrelenting.
How Common Is Endometriosis?
According to the Cleveland Clinic and MedicalNewsToday, endometriosis affects an estimated 1 in 10 people with a uterus during reproductive years. Despite how common it is, many are misdiagnosed or dismissed for years.
Signs & Symptoms You Should Not Ignore
The symptoms vary widely. Some experience extreme pain, while others have mild symptoms but still have advanced disease.
The most common symptoms include:
1. Pelvic pain
- Pain before, during, or after periods
- Pain that interferes with daily life
- Pain that feels deeper than “normal cramps”
2. Pain during or after sex
Deep pelvic pain during intercourse is a major indicator of this condition.
3. Painful bowel movements or urination
Especially worse around your period.
4. Heavy or irregular periods
Some may experience long periods, heavy flow, or spotting between cycles.
5. Bloating, nausea, and fatigue
Endometriosis can mimic IBS (irritable bowel syndrome) symptoms.
6. Difficulty getting pregnant
Endometriosis is found in 20–50% of people struggling with infertility
7. Lower back pain
Especially during menstruation.
Why Does Endometriosis Cause So Much Pain?
This pain is not in your head and it’s not “just bad period cramps.”
Endometriosis tissue:
- Bleeds where it shouldn’t
- Causes inflammation
- Creates scar tissue
- Can bind organs together
- Triggers nerve pain
Whether the pain is sharp, dull, stabbing, or persistent, it is considered one of the most painful gynecological conditions.
What Causes Endometriosis?
Doctors still don’t know the exact cause, but major theories supported by research include:
1. Retrograde menstruation
Menstrual blood flows backward through the fallopian tubes into the pelvic cavity, carrying endometrial-like cells that implant.
2. Immune system problems
A weakened immune system may fail to clear the misplaced tissue.
3. Cellular transformation
Cells outside the uterus may spontaneously turn into endometrial-like tissue.
4. Hormonal influences
High estrogen levels may encourage endometriosis growth.
5. Surgical scar implantation
After surgeries like C-sections, endometrial cells can attach to the scar.
6. Genetics
Endometriosis tends to run in families.
Risk Factors
- You may be more likely to have endometriosis if:
- You started periods early
- You have short menstrual cycles
- Your periods are heavy or last longer than 7 days
- You have never given birth
- You have a family history
- You have reproductive tract abnormalities
How Endometriosis Affects Fertility
Not everyone with endometriosis struggles with fertility, but many do.
Endometriosis can impact fertility by:
- Blocking fallopian tubes
- Causing inflammation that affects egg quality
- Reducing ovarian reserve
- Disrupting ovulation
- Causing adhesions around reproductive organs
According to the Mayo Clinic, up to 50% of people with infertility may have endometriosis.
But pregnancy is still very possible, especially with early diagnosis and treatment.
How Is Endometriosis Diagnosed?
Endometriosis can be difficult to diagnose because symptoms overlap with other conditions.
Doctors may use:
1. Pelvic exam
To check for cysts, nodules, or scarring.
2. Ultrasound
Useful for spotting endometriomas (ovarian cysts).
3. MRI
Detailed imaging to identify deep lesions.
4. Laparoscopy (definitive diagnosis)
A surgeon inserts a small camera through the abdomen to directly see and sometimes remove endometriosis tissue.
Treatment Options
Treatment depends on your symptoms and whether you want to become pregnant.
1. Pain Medication
Over-the-counter anti-inflammatories (NSAIDs) may reduce discomfort.
2. Hormonal Therapy
Used to reduce or stop menstruation, which slows endometriosis growth.
Options include:
- Birth control pills
- Progestin therapy
- Hormonal IUD
- GnRH agonists or antagonists
3. Surgery
Laparoscopic surgery can:
- Remove endometriosis tissue
- Remove adhesions
- Drain or remove cysts
Surgery may improve pain and fertility.
4. Fertility Treatment
If pregnancy is the goal, options include:
- Ovulation induction
- IUI
- IVF
5. Lifestyle Support
While lifestyle changes do not cure endometriosis, they can help reduce symptoms:
- Anti-inflammatory eating
- Gentle exercise
- Heat therapy
- Stress reduction
- Adequate sleep
These methods help manage inflammation and pain.
Living with Endometriosis
Endometriosis is a chronic condition. Symptoms may come and go, and flare-ups are common. The goal of treatment is to manage pain, protect fertility, and maintain a good quality of life.
Many people find it helpful to track:
- Pain levels
- Diet changes
- Period patterns
- Triggers
- Bowel or urinary symptoms
Understanding your own patterns can help you make informed decisions and communicate more effectively with your doctor.
When Should You See a Doctor?
Seek medical advice if:
- Period pain stops you from working or performing daily activities
- You experience severe pain during intercourse
- You have difficulty getting pregnant
- Your cramps worsen over time
- Pain medications no longer help
These are not “normal” symptoms, they deserve attention.
Final Thoughts
Endometriosis is a real medical condition, not something to brush off as “bad period pain.” With proper diagnosis, treatment, and symptom management, many people find relief and regain control of their lives.
The key is awareness. The sooner endometriosis is understood and recognized, the sooner effective treatment can begin.
If you suspect you may have this conition, talk to a healthcare provider. Your pain is valid, and options exist to help you feel better.